Ear Eczema
Ear eczema can be an extremely irritating and, at times, painful condition. It can range from slight dryness of the pinna (the visible, projecting part of the ear) to extensive skin loss and soreness, as well as infection of the external and internal parts of the ear.
Eczema can affect the entire ear including the ear lobes, conchal bowl (the area outside the ear-hole), the ear opening (meatus), ear canal (also known as the external auditory canal – the part of the ear which leads to the ear drum) and the ear drum itself (also known as the tympanic membrane).
The ear-folds, backs of the ears and the area where the ears meet the face are also common areas for eczema. Inflammation of the ear canal is called otitis externa and has a number of causes.
It is important to focus on the prevention and control of otitis externa as, if left untreated, eczema or infection in this area can worsen and spread outwards to the pinna and surrounding skin.
Types of ear eczema
There are a number of causes of ear eczema and it is always best to consult your doctor if you think you may have it, in order to get effective treatment and prevent flare-ups. Several different types of eczema may affect the ear.
Atopic eczema
The ears and skin behind the ears are frequently affected in people with atopic eczema. As with other areas of the body, the eczematous skin is red, dry and itchy, and can easily become infected, especially if scratched and the skin is broken.
A common area for ear eczema in people with atopic eczema is at the junction between the ear lobe and the face.
Eczema in this area can cause painful cracks (fissures) in the skin, which can then easily become infected. Sometimes eczema can affect the whole of the pinna and track down the ear canal.
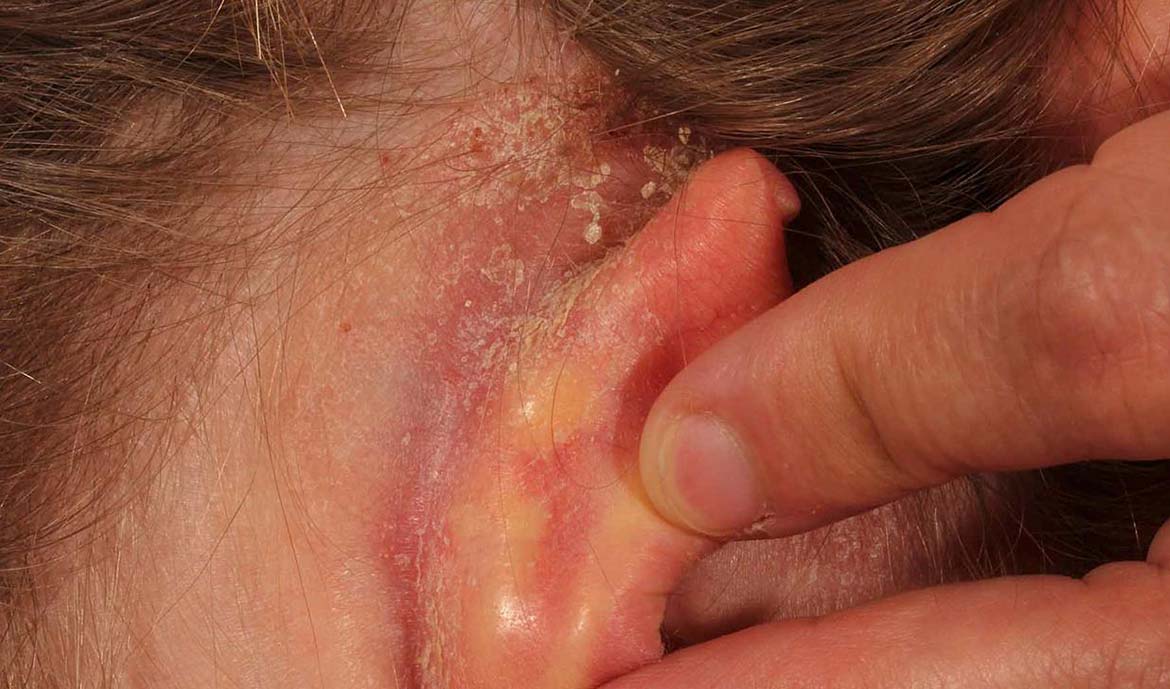
Seborrhoeic eczema (dermatitis)
Seborrhoeic eczema affects areas of the body where there are sebaceous glands, including the ears, scalp, face and trunk. In its mildest form, seborrhoeic dermatitis simply causes scaling and redness at the entrance to the external ear canal. In its more severe forms, redness and crusty cracks develop in the ear folds and extend to the external ear, and the scalp and neck can also be affected.
Asteatotic eczema
This type of eczema affects older people. The exposed ear is vulnerable to changes in climate, which leads to dry, scaly and itchy skin causing asteatotic eczema. Aggravating factors include over-washing, cold or windy weather, heating, low humidity indoors and air-conditioning.
Contact dermatitis
The external ear is commonly affected by both irritant and allergic contact dermatitis. Irritant contact dermatitis results when the skin’s surface is irritated by a substance that causes the skin to become dry, red and itchy.
Examples of substances that can cause irritant contact dermatitis around and inside the ears are shampoos, hair gels, hair spray, perm solution, hair colourants and perfume. Allergic contact dermatitis may appear as a result of your body reacting to a particular substance to which you are allergic.
Everyday items that can cause allergic contact dermatitis around and inside the ears include the following:
- Products used for the hair and scalp (eg shampoo, conditioner, gels, hairspray, hair colourants, perm solution, hair pins and grips, hairnets and bathing caps)
- Earrings and studs, especially those containing nickel
- Plastic, rubber or metal ear appliances (eg hearing aids and moulds, spectacles, head- and earphones, mobile phone/ipod receivers and earplugs)
- Objects used to clean or scratch the ear
- Cosmetics and toiletries (eg make-up, perfume and soap)
- Topical medicaments (eg ointments, creams and gels)
- Allergens transferred to the ears via the fingers (eg nail varnish and plant resin from poison ivy, oak).
Ear piercing
Ear piercing does not cause ear eczema, but problems can occur later on as a consequence of wearing earrings or studs. Nickel allergy is very common and the chance of this developing is greatly increased if you have your ears pierced and if anything made even partly from nickel is worn in or on the ear.
If you definitely have a nickel allergy, wear only ‘hypo-allergenic’ jewellery or that made of 18-carat gold, pure sterling silver, platinum or good-quality stainless steel. Foreign silver, rolled gold, white gold and gold plating should be avoided.
Pierced ears can become infected, particularly just after piercing. Make sure you go to a reputable ear-piercing technician to get your ears pierced, and bathe them frequently afterwards with a weak antiseptic solution until they stop weeping.
Treatment of ear eczema
Treatment of ear eczema will depend on the cause and type of eczema, which will need to be diagnosed by your GP. Possible treatments that you may be prescribed are listed below.
For atopic, seborrhoeic or asteatotic eczema, apply a medical emollient frequently to the affected areas. You may be prescribed a topical steroid on sore areas behind the ears, and in their folds. If you have seborrhoeic dermatitis, a topical steroid combined with an antifungal may be prescribed.
Apply your topical treatments to the affected area by using a cotton bud to gently paint on your cream or ointment around the ear pinna and the opening to your ear canal (ear meatus). Do not push the cotton bud into your ear.
If you have eczema inside the ear canal, you will need steroid drops, which will be prescribed by your GP.
If allergic contact dermatitis is suspected, you may be referred to a Dermatologist to help diagnose what you are allergic to so that you can avoid it in the future. The Dermatologist will usually recommend patch testing.
Cleaning of the ears and self-care
You can very gently wash the inside of your outer ear with water or preferably an emollient wash. You can also use a damp cotton bud very gently in the bowl area of your ear but do not insert it into the ear canal. Never try to wash further into the ears – you can damage the skin of the ear canal by doing this.
After washing, dry your ears thoroughly – using a warm (not hot) hairdryer is a good way to ensure your ears are dry. Avoid scratching the inside of your ears, especially with matches or hair grips – not only can these damage your ear canal skin or drum, but they may cause an allergic reaction after continuous use.
The use of ear candles is not advised as there is no evidence to suggest that they work, and they can cause damage to ears. If you go swimming, use ear plugs. You can get custom-made ear moulds to fit your ears – they are like the moulds used as hearing-aids. Ear moulds can be made and fitted at hearing-aid centres or at private audiologists.
Olive oil may sometimes be recommended for moisturising around the ear pinna and loosening wax. However, there is medical research evidence showing that olive oil damages the skin barrier. Instead, we suggest that an emollient cream/ointment is applied to treat dry skin around the ears and in the entrance to the ear canals, and refined petroleum oil (unfragranced baby oil) or sunflower oil is used for softening ear wax (but consult first with a healthcare professional).
Water is not recommended, nor are wax softener products bought from chemists as they may encourage the build-up of debris and cause more inflammation and irritation.
Infected ear eczema
Skin affected by eczema and dermatitis can become infected, usually by bacteria, especially if the skin surface is broken due to dryness and scratching. This is similar to eczema infections in other areas of the skin.
Ear eczema that becomes infected can encourage a build-up of wax, skin scales and hair in the ear canal, which can lead to blockage and cause temporary deafness. Infected eczema and ear infections can also result when the ears are wet for long periods of time – for instance if you swim a lot and if you leave your ears damp after swimming or washing your hair, your chances of an ear infection are further increased. Pressure from hearing aids and earpieces can also encourage ear infection so try to ensure they are a comfortable fit.
Symptoms of infection inside the ear include earache, itching, pain, redness, weeping, swelling and an unpleasant smell or dirty-coloured discharge (often yellow or green) from inside the ear. If you have any of these signs, make an appointment to see your GP. Please note: ear discharge that is clear is normal if you have ear eczema, especially when eczema is active (weepy eczema).
If you think your ear eczema is infected, see your GP. You may be prescribed a ‘combination’ preparation containing a mixture of antibiotic and topical steroid for bacterial infections, or an antifungal and topical steroid for fungal infections. You should complete the course of treatment.
Aural toilet by healthcare professionals
A build-up of wax and the flaky skin from patches of eczema can produce a lot of ‘debris’ in the ear canal and this can easily get infected, especially when water is present. So prevention of ear infection is key.
Manual cleaning of the ear by a healthcare professional is called ‘aural toilet’ and is often recommended to remove the debris and scale that can build up in the ear canal. It is done under a microscope, either using a pick or hook (Johnson Horne probe) or using microsuction, an electric suction system.
Microsuction is also recommended if ear wax is truly impacted, and is considered safer and definitely better than flushing the ears with water, especially for people with ear eczema.
Although many GP practices offer ear syringing and/or ear irrigation (an electronic machine for washing the ears) to remove ear wax, water-based methods are not recommended for people with ear eczema, unless it is very mild. Sometimes regular aural toilet is recommended (once or twice a year) to prevent wax and eczemadebris build-up.
Aural toilet can be performed by aural care nurses/technicians, or sometimes by specially trained practice nurses. Ask your GP for a referral to an aural care service or to a private audiologist.
In summary
Ear eczema can be an extremely irritating condition and since it is difficult to look into the ears without specialist equipment, it is often hard to know what is going on, particularly in the case of young children.
If the ears become uncomfortable, don’t ignore it – it is always best to see your GP/healthcare professional, who can use a special torch to look inside. Often this will reveal the cause of ear discomfort and the problem can then be resolved, using one of the many treatments available for ear eczema and ear infections.
Information contained in this article was obtained from the Ear Eczema Info Sheet published by the National Eczema Society
It is not the policy of the Eczema Association of Australasia Inc to recommend or endorse any product or treatment.
It is part of the role of the Association to provide information on a wide range of products and treatments to keep those involved with eczema as fully informed as possible as to all options available. For medical advice, consult your health professional.




