Red Skin Syndrome (TSW) is NOT eczema
I joined the Eczema Association of Australasia after becoming desperate for an end to my itchy, red skin. I was first diagnosed with eczema around the age of 20 and prescribed a mild steroid cream for the rash on my chest. The rash cleared and the unfinished tube of cream sat idle in my bathroom cupboard for years. In my late twenties and thirties, I occasionally developed a small patch of dry skin, which I sometimes treated with a topical steroid cream or with a non‐steroidal emollient. It wasn’t until my early forties that my skin rash become problematic. It started in my ears – insane itchiness which I constantly aggravated. I was prescribed steroid drops for it. Then my hands started getting itchy. I used elecon lotion on them. Then my hands would clear, but my legs would break out, or my back. I took a course of prednisone because I needed to have a break from the constantly sore, itchy, red skin that would break out on various parts of my body. The prednisone worked a treat – for a while. After a few months though, a rash started to re‐appear on my legs, then my hands. I went back to using elocon. I started the next year as usual, by trying to only use elocon as needed, rotating through four or five days on and a couple of weeks off as I knew it wasn’t safe to use it continuously. But always, after not using it for four or five days, the rash would come back. In July that year I developed a cluster of pimple‐like bumps on one cheek. After two weeks, more of these pimples appeared on the other cheek. Then, overnight, my face became red, swollen and sore to touch. My dermatologist diagnosed steroid‐induced rosacea and said it was due to touching my face with fingers that held traces of elocon. I went home and resolved not to use elocon at all, anywhere
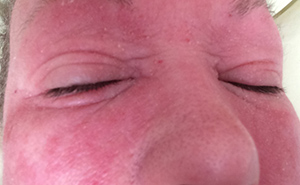
Within a few weeks, the redness and itchiness spread. My neck had big, red, sore lumps on it and my face and neck were insanely itchy. I begged for another course of prednisone. My dermatologist obliged and I had five blissful days of clear skin. Then, as I tapered off the medication, my neck started to get red and itchy again. And my face. And my arms. And my hands. I stopped the prednisone and the next day (day two of steroid withdrawal) my face was burning hot and had starting weeping an oozy, yellow liquid. My eyes were swollen, my stomach was itchy, my legs were getting itchy behind my knees. By day 3, my armpits were hot, red and sore to touch. By day five, I had red, hot, itchy skin all over my body and yellow ooze all over my face, neck and arms. I had oedema in my hands and arms.
It was at this time that I joined the EAA – and so began my journey of being saved from this so‐called “eczema” hell. Within a week of joining, I received my first newsletter, which included an insert from a man called Peter from Western Australia. Peter spoke about his wife and their journey to end her suffering. He mentioned a website established by a woman called Kelly Palace. I checked out these websites and realised that what I had was not eczema – it was Red Skin Syndrome – a condition caused by steroid withdrawal.
I went back to my dermatologist with this information, plus a published research paper on the topic by a highly regarded dermatologist from California, Dr Marvin Rapaport but my dermatologist was not interested in this diagnosis. I decided to go it alone (well, I had fantastic support from others suffering from Red Skin Syndrome, which I accessed via a forum set up by Kelly Palace – a google group called Cure Eczema by Stopping Steroids. I never would have got through it without them).
The next three months were hell. I developed severe oedema in my legs and feet, was largely bedridden, (I couldn’t wear shoes, let alone any clothes other than a sarong and old t‐shirt). My skin exuded, burned, flaked and itched. I shivered uncontrollably. My lymph nodes grew to the size of grapes. My legs ached, it was painful to walk. I looked a mess. I was a mess. I cried. A lot.
I kept a diary of my progress (although, for a long time it didn’t feel like progress) and took many photos along the way. I checked into the forum daily and drew enormous support from others going through the same nightmare as me. On the forum, I learned of others, adults and children alike (children just like Holly) who had made a full recovery and now had beautiful skin without using steroids.
In months four and five, the oedema slowly receded, the weeping eventually stopped and I was left mainly with itchiness to deal with and perpetually pink skin. Thankfully, my energy levels returned and I started to get active again and enjoy life.
It is now eight months since I ceased using steroids and my skin is finally showing signs of recovering from topical steroid abuse. It has its normal colour back, my arms still feel a bit dry and my neck gets itchy occasionally. The skin on my legs and feet is still damaged from daily scratching but is healing slowly.
Red Skin Syndrome is an awful and completely preventable condition that has not only affected my skin, but my whole life and that of my loved ones. It has taken me to the darkest depths of despair but also taught me to be patient and persevere. The healing process is a slow and painful one, but thankfully, a successful one for those who can endure it. I will never use topical steroid creams again and I know that my skin will continue to soften and recover until, one day soon, I will have soft, smooth, silky skin all over.
For more information visit ITSAN www.itsan.org
Following is a link to a book on TSW written by sufferer Kelly Barta about her journey which is very interesting for anyone who thinks they may be suffering from TSW: www.amazon.com/Kelly-Barta/e/Book
It is not the policy of the Eczema Association of Australasia Inc to recommend or endorse any product or treatment.
It is part of the role of the Association to provide information on a wide range of products and treatments to keep those involved with eczema as fully informed as possible as to all options available. For medical advice, consult your health professional.




